Wisdom Teeth
Why did humans develop wisdom teeth? Do they need to be removed? Read on to find out more...
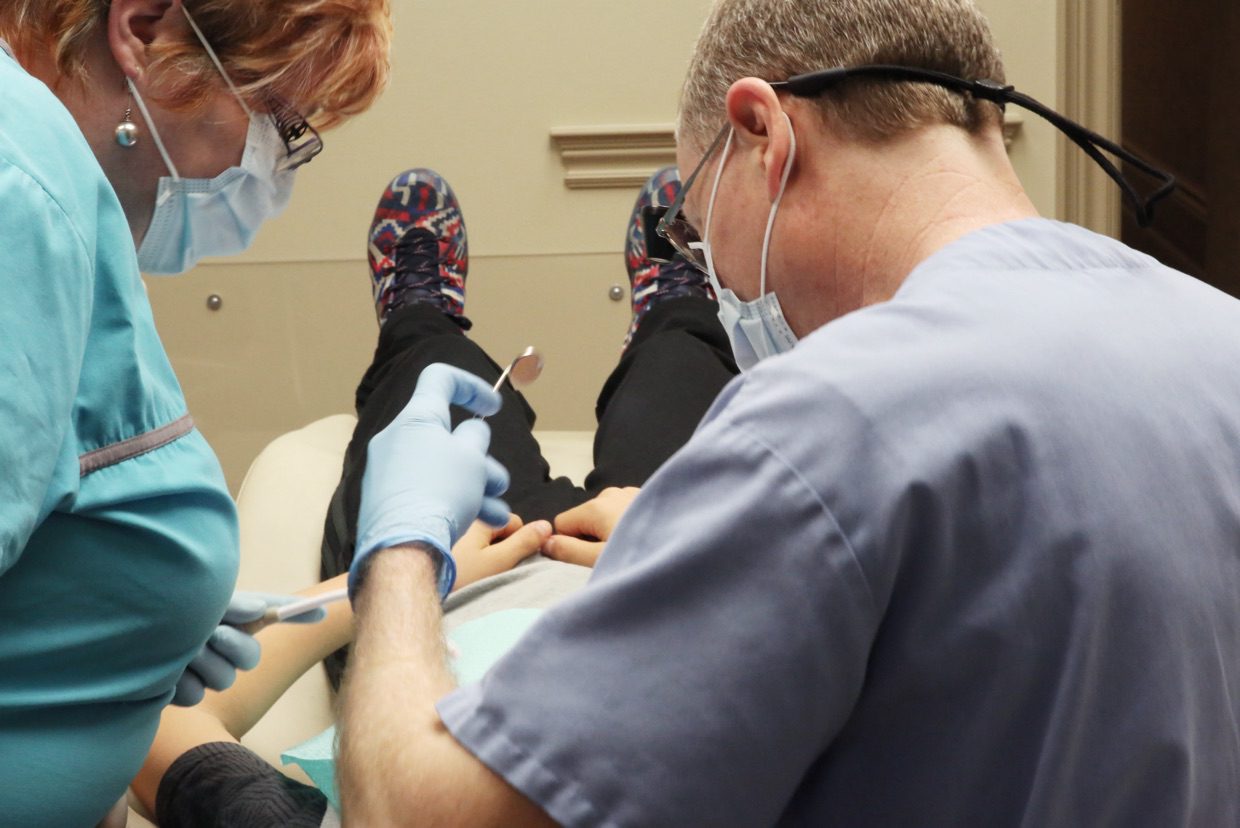
To remove, or not to remove?
When considering wisdom teeth, it is likely to encounter a debate on whether to remove wisdom teeth, or take a "watchful waiting" approach. So how might we make the choice between proceeding with the surgical removal of wisdom teeth, or, avoiding the surgery? The answer will lie in the evaluation of the current state of health of the individual patient and their individual philosophy (or that of their supporting family members like mom or dad), and, of course, the findings from a specific dental examination. The latter exam focusses on the clinical conditions of the wisdom teeth, their surrounding bone and gum tissues, and the revealing X-Ray information.
General Background: The four teeth at the very back of the jaw, called the third molars, generally start to 'show up' or shift at 16 to 25 years of age (although the variability can be quite considerable). Of course, the wisdom teeth may remain buried well below gums and bone, or they may break through the gums in part, or they can even fully emerge in to the mouth. Unfortunately, with no bias from the dental office, very often we see clear indications that there is not enough room in the jaw for their useful eruption and function -- a such, they may be considered impacted. Such positioning of poorly located wisdom teeth can lead to accumulation of plaque, risk gum swellings, decay, and long-term problems such as progressive gum disease. These unwanted conditions not only effect the wisdom teeth, the very support and integrity of the adjacent adult second molars may be compromised. This leads many dentists suggest removing them despite no apparent diseases in the teeth at a young adult age.
To add further consideration to the above, the following consequences generally increase with age and wisdom teeth -- harder bone that makes removing wisdom teeth more difficult, increasing discomfort from the removal and slower healing. It is worthwhile noting here that research studies found insufficient data to suggest that taking out wisdom teeth reduced crowding of the remaining teeth (2012 Cochrane review of randomized clinical trials over five years).
Included in the decision to remove wisdom teeth is the consideration of the procedure complexity. Many factors may be weighed with a view to the 'pros' and 'cons' about tooth position, the proximity to other structures (nerves, sinuses, adjacent teeth, etc.).
Risks
Unfortunately, risk is part of any surgery, even the most routine. Risks are discussed and are taken seriously in every circumstance. When weighing the risks of wisdom tooth extraction, we analyze the question of "What's the relative benefit?" Both dental disease surrounding existing wisdom teeth and the consideration of using predictions will prove to help with the assessment of risks. While some risks are a natural consequence of the tooth extraction surgery, there are other rare complications. It may be anticipated and expected to manage pain, normal bleeding/oozing, bruising, transient restricted jaw opening, And in rare cases, nerve injury leaves people with permanent lip, tongue and cheek numbness after removing wisdom teeth, according to the American Public Health Assn.
Local Anesthetic and Sedation
There is no doubt that local anaesthetic ("dental freezing") is the pillar of pain control during wisdom teeth extractions. There is also no questioning the degree of apprehension which accompanies these surgical procedures. Removing wisdom teeth involves management of the patient's concerns about physical surgery and psychological experience. Perhaps, the most optimal state with the greatest assurance of safety is found when the teeth can b removed with a combination of local anaesthetic in conjunction with a conscious sedation technique. The latter form of sedation anaesthesia is sometimes referred to as a "twilight sleep" or moderate sedation. Administering these modalities, the patient is relaxed, tranquil, vaguely aware of their environment, yet, able to communicate with with the dentist and staff. The local anaesthetic affords the pain control and the patient avoids adding the risk of general anaesthesia — which makes the patient unconscious and eliminates the natural protective airway reflexes.
Keeping teeth
But there also are risks to keeping wisdom teeth, including gum infections or the potential for emergency surgery, says Dr. Thomas Dodson, a professor in oral and maxillofacial surgery at the University of Washington. Recent studies have shown that third molars can be unpredictable, he says. About 60% of his patients choose to have their wisdom teeth removed, he says. For those who keep their teeth, close monitoring by dentists and careful care by their owners are required. Scott Tomar, a professor of community dentistry and behavioral science at the University of Florida, considers removing healthy wisdom teeth no different than removing a healthy appendix just in case it might burst. "I don't know of any other surgical treatment still done in the United States where we prophylactically do an invasive surgical procedure unless there's pretty strong evidence supporting it. We've abandoned that idea long ago."
The theory behind wisdom teeth
Why did humans develop wisdom teeth — apparently called that because they emerge after we've accumulated a bit of wisdom? Scientists theorize that early humans once put their wisdom teeth to good use. That's because the human diet was largely roots, tough meats and raw food. Think jerky — morning, noon and night. With these hard-to-eat foods, it meant the human jaw worked much harder to grind up a meal before swallowing. The extra teeth helped get the job done. According to scientists, at one time the jaw was larger, something that gave ample room for these often-misunderstood molars to thrive.